For years, Lifestyle Medicine (LM) has been championed for its ability to prevent, treat, and even reverse chronic disease. But a new qualitative study published in BMC Health Services Research adds a compelling dimension to the conversation: LM doesn’t just transform patient health—it may also protect clinicians’ well-being.
At a time when healthcare worker burnout is reaching crisis levels globally, this finding is more than interesting. It’s urgent.
Drawing on in‑depth interviews with 42 healthcare workers across five U.S. health systems, the study explores how implementing LM affects both patient outcomes and practitioner experience. The result is a conceptual model showing that LM can meaningfully reduce burnout by enhancing professional joy, restoring a sense of purpose, and improving the clinical environment.
For Whole Food Living readers—many of whom work at the intersection of lifestyle, health, and community—this research offers a powerful reminder: when we shift the focus of healthcare toward root causes and human connection, everyone benefits.
Burnout matters
Burnout is more than fatigue. The World Health Organisation defines it across three dimensions:
- Exhaustion
- Detachment or cynicism
- Reduced sense of professional efficacy
These symptoms don’t just harm clinicians—they ripple outward, affecting patient care, staff retention, and the overall functioning of health systems.
Traditional burnout interventions often focus on individual resilience. But the study highlights something different: when the work itself becomes more meaningful, energising, and aligned with personal values, burnout naturally declines.
Lifestyle Medicine appears to offer exactly that.
Dramatic patient improvement
One of the strongest themes emerging from the interviews was the sheer joy clinicians experienced when witnessing dramatic patient improvements. Many described patients reducing medications, reversing diabetes markers, healing chronic wounds, or regaining mobility.
One administrator shared the story of a patient whose HbA1c dropped from over 12 to 5 after participating in an LM program—an outcome that would be remarkable under any model of care.
For clinicians accustomed to managing chronic disease rather than resolving it, these transformations were deeply energising. They restored a sense of professional efficacy—one of the core antidotes to burnout.
As one physician put it, LM “completely changed my perspective on what it means to be a doctor.”
Patient empowerment
Another major theme was patient empowerment. LM shifts the dynamic from passive treatment to active partnership. Patients learn skills, set goals, and take ownership of their health.
A psychologist interviewed in the study described LM as “more patient‑centered… it empowers the patient. It puts them in the driver’s seat.”
This shift doesn’t just help patients—it reduces emotional strain on clinicians. When patients feel engaged and hopeful, clinicians feel less drained and more connected.
And patient satisfaction? According to participants, it skyrockets. Some clinics reported patient experience scores “off the charts,” with patients returning and bringing friends.
In a healthcare landscape where dissatisfaction is common, this kind of positive feedback loop is rare—and precious.
Moral alignment
Many clinicians in the study expressed a profound sense of moral alignment with LM. They felt it represented the way medicine ought to be practised: addressing root causes, prioritising prevention, and treating patients as whole people.
One physician said, “Talking about lifestyle should always come first before we quickly pull out the prescription pad.”
This alignment between values and practice is a powerful buffer against burnout. When clinicians feel they are doing the work they were called to do, their sense of meaning increases—another key protective factor.
LM programs often foster collaborative, like‑minded teams. Clinicians described environments in which colleagues supported each other’s healthy habits, enthusiastically shared ideas, and worked toward a common mission.
Some health systems even implemented LM wellness initiatives for staff, helping clinicians improve their own nutrition, movement, sleep, and stress management. These changes not only improved personal well-being but also strengthened clinicians’ belief in the model they were delivering.
As one practitioner said, “It has helped me be a better person… we help each other eat better [and] set boundaries so we’re not overworking.”
This sense of community and shared purpose directly counters the isolation and exhaustion that fuel burnout.
The challenges
The study did include one dissenting voice: a dietitian who felt burned out from repeatedly advocating for plant‑based nutrition in a system where not all departments were aligned. The emotional labour of “pushing the message” without institutional support was draining.
This highlights an important caveat: LM reduces burnout most effectively when implemented system‑wide. Fragmented or unsupported efforts can have the opposite effect.
Researchers developed a model showing how LM influences the three components of burnout:
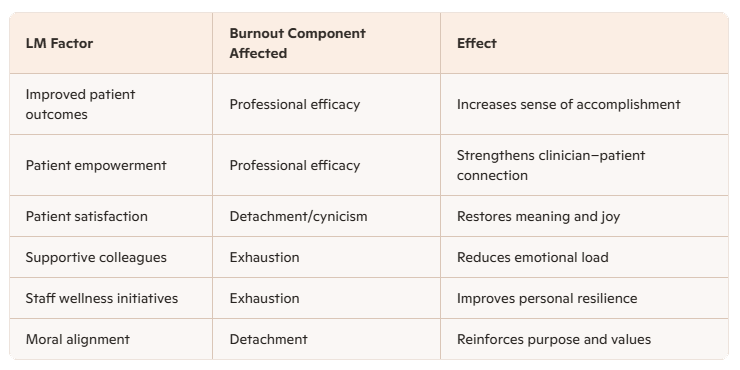
Together, these factors create a “virtuous cycle” where clinicians feel more effective, more connected, and more energised.
Future of healthcare
Lifestyle Medicine is still a relatively young speciality, formally recognised by the American Medical Association only in 2024. But its potential is enormous.
If LM can simultaneously:
- improve patient outcomes,
- reduce healthcare costs,
- increase patient satisfaction, and
- protect clinician wellbeing,
then it supports all four pillars of the “quadruple aim” of healthcare. In a world where chronic disease is rising, and clinician morale is falling, LM offers a rare and hopeful path forward.
The takeaway
This study reinforces what many in the Whole Food Living community already know: when healthcare focuses on lifestyle, connection, and empowerment, the benefits extend far beyond the patient.
Lifestyle Medicine doesn’t just heal bodies. It heals the practice of medicine itself.





